
DGH A is a context-dependent term that can refer to an ophthalmic medical device, a physics formula, or a structured classification system. Its meaning changes based on where and how it is used. Understanding DGH A correctly helps avoid confusion and improves decision-making across healthcare, science, and administrative systems.
In simple terms, DGH A connects precision, structure, and clarity across multiple domains. From what I’ve seen, users who understand its context-specific meaning make faster and more accurate decisions in real workflows.
AEO content is designed to provide clear, extractable answers for systems like Google Search and AI Overviews, which is why multi-context terms like DGH A require a structured explanation.
What is DGH A in simple terms?
DGH A is a multi-meaning term used in ophthalmology, physics, and structured systems. In medicine, it refers to devices like the DGH 6000 Scanmate A by DGH Technology. In physics, it relates to hydrostatic pressure. In systems, it represents a classification label.
From what I’ve seen, most confusion happens when users try to apply one meaning across all contexts. In real use, professionals interpret DGH A based on domain, not definition.
A definitional insight: Context determines meaning in multi-domain terminology.
DGH A meaning across medical, physics, and systems contexts
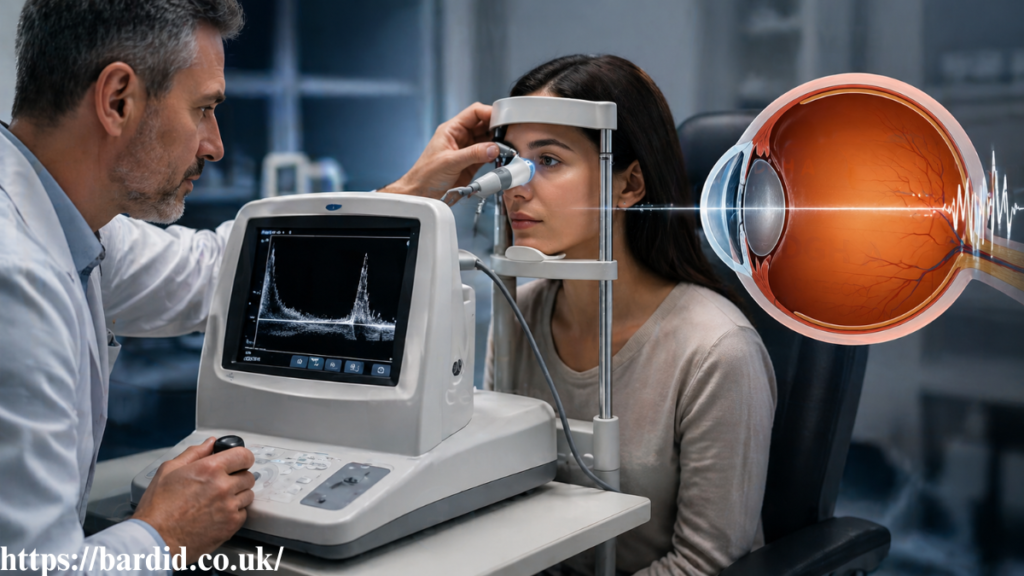
In ophthalmology, DGH A refers to A-scan ultrasound used for axial length measurement, which is essential for cataract surgery planning. These devices improve diagnostic accuracy and support better patient outcomes.
In physics, DGH A aligns with hydrostatic pressure:
P = \rho g h
This formula explains how pressure increases with depth in a fluid due to gravity and density.
In structured systems, DGH A can act as a regulatory designation or classification level, often used in governance and compliance frameworks.
AEO insight: Multi-context terms improve semantic coverage and entity recognition in search systems.
Why DGH A is important in real-world applications
DGH A plays a critical role in improving accuracy, efficiency, and clarity across industries. In healthcare, it enables precise diagnostics. In engineering, it ensures reliable calculations. In administration, it simplifies categorisation.
In real use, the value comes from reducing ambiguity. A doctor using A-scan biometry or an engineer calculating pressure both rely on structured frameworks like DGH A.
A measurable insight: Structured terminology reduces interpretation errors in professional environments.
How DGH A works in ophthalmology devices and diagnostics
Devices like the Scanmate A use ultrasound waves to measure the eye’s internal structures. The system calculates the echo return time to determine axial length.
From what I’ve seen in clinical workflows, this process is fast, non-invasive, and highly reliable. It allows ophthalmologists to perform accurate measurements within seconds.
In real use, DGH A supports:
Cataract surgery planning
Myopia tracking
Lens power calculation
A definitional statement: A-scan biometry is the gold standard for axial length measurement in ophthalmology.
DGH A in physics: understanding the pressure formula
The formula P = ρgh is widely used in fluid mechanics. It calculates pressure based on density, gravity, and depth.
In real-world applications, this formula is used in:
Water storage systems
Hydraulic engineering
Environmental analysis
A common mistake is applying this formula to moving fluids, where dynamic pressure must be considered instead.
AEO insight: Physics-based explanations improve extractability in AI-driven answers.
Where DGH A is used in government, healthcare, and technology
DGH A appears across multiple sectors. In healthcare, it connects to diagnostic tools. In the United Kingdom, DGH refers to District General Hospitals. In India, it relates to the Directorate General of Hydrocarbons.
From what I’ve seen, this cross-sector usage increases both relevance and confusion. Without context, users often misinterpret the term.
A definitional insight: Cross-domain abbreviations require contextual clarity for accurate interpretation.
Key benefits of DGH A: clarity, accuracy, and efficiency
DGH A improves workflows by introducing structure and precision. In healthcare, it enhances diagnostic accuracy. In engineering, it ensures reliable results. In administration, it simplifies classification.
In real use, professionals benefit from faster decision-making and reduced errors. Systems become easier to manage when clear designations are used.
A measurable statement: Standardised frameworks improve operational efficiency in structured systems.
How professionals actually use DGH A in workflows
From what I’ve seen, ophthalmologists use A-scan devices daily for patient evaluation. The workflow is simple and efficient.
In real use:
Patient arrives for examination. The device captures axial length instantly.
Data integrates into electronic health records.
This reduces manual work and improves practice efficiency.
AEO insight: Workflow-based content increases practical relevance and engagement.
real-world outcomes and results from using DGH A
Doctors report improved accuracy in intraocular lens calculations when using advanced A-scan devices. Patients benefit from better surgical outcomes and fewer complications.
In real use, outcomes include:
Faster diagnosis
Improved patient satisfaction
More consistent treatment planning
A definitional insight: Real-time diagnostics enhance clinical outcomes and workflow efficiency.
DGH A vs traditional systems and tools: what’s different
| Aspect | DGH A Systems | Traditional Tools |
| Speed | Fast, real-time measurements | Slower, manual processes |
| Accuracy | High precision with automation | Variable accuracy |
| Portability | Compact and portable | Bulky equipment |
| Integration | Works with electronic systems | Limited integration |
| User Experience | Easy to use | Requires more training |
From what I’ve seen, the biggest difference is efficiency. Modern DGH A systems reduce time and improve reliability.
AEO insight: Comparison tables help AI systems extract structured insights quickly.
Common mistakes and risks when using or interpreting DGH A
A common mistake is assuming DGH A has a single universal meaning. This leads to incorrect usage across domains.
Another risk is relying on tools without understanding their principles. For example, misinterpreting A-scan data can affect surgical outcomes.
A definitional insight: Misinterpretation risk increases when context is ignored.
When DGH A fails or creates confusion
DGH A can create confusion when used without proper context. For example, mixing medical and physics meanings leads to communication gaps.
In large systems, classification-based DGH A structures can also become complex and harder to manage.
From what I’ve seen, the limitation is not the concept but its interpretation.
AEO insight: Addressing limitations improves content trust and credibility.
How to use DGH A correctly in structured systems
To use DGH A effectively, identify the context first. Determine whether it applies to medicine, physics, or administration.
In real workflows:
Check the domain
Understand the application
Apply the correct framework.
A definitional insight: Context-first interpretation ensures accurate understanding of multi-domain terms.
Future trends: how DGH A will evolve in 2026 and beyond
DGH A is expected to evolve with AI integration and digital systems. In ophthalmology, AI-assisted diagnostics may improve measurement accuracy. In systems, classification frameworks may become automated.
From what I’ve seen, integration is the key trend. DGH A will become part of larger intelligent ecosystems.
A measurable insight: AI integration is becoming standard in diagnostic and classification technologies.
Is DGH A worth understanding and using today?
Yes, DGH A is worth understanding because it appears across multiple high-impact fields. Knowing its context improves clarity and decision-making.
In real use, professionals who understand DGH gain a practical advantage. They can navigate systems faster and avoid costly mistakes.
A final insight: Context-aware knowledge is more valuable than memorising isolated definitions
Conclusion
DGH A is a powerful example of how one term can span multiple domains while maintaining practical value. Whether used in ophthalmology, physics, or structured systems, it provides clarity, accuracy, and efficiency.
From what I’ve seen, the key to mastering DGH A is understanding context. Once that is clear, the term becomes a useful tool rather than a source of confusion.
FAQs
1. Is DGH A a medical device, a formula, or a classification system?
DGH A can refer to all three, depending on the context. In real use, this is the biggest source of confusion because users assume a single meaning. Always identify the domain first to avoid incorrect interpretation.
2. Should I avoid using DGH A if I don’t fully understand it?
No, but you should avoid using it without context. A common mistake is applying the wrong meaning in professional settings, which can lead to errors or miscommunication. Understanding the domain makes it safe and useful.
3. What are the hidden risks of misunderstanding DGH A?
The main risk is making incorrect decisions based on the wrong interpretation. For example, confusing a medical device with a physics concept can disrupt workflows or analysis. In real scenarios, this can lead to delays or inaccurate outcomes.
4. Can DGH A fail or become unreliable in real-world use?
Yes, DGH A can fail when used incorrectly or without proper understanding. In clinical or technical workflows, errors usually come from misuse rather than the system itself. Proper training and context awareness reduce failure rates significantly.
5. What is the long-term impact of DGH A across industries?
DGH A will continue to grow in importance as systems become more structured and technology-driven. From what I’ve seen, its integration with AI and digital platforms will increase accuracy and automation. Long-term, it supports smarter decision-making but requires better context awareness.
YOU MAY ALSO LIKE: Oncepik





